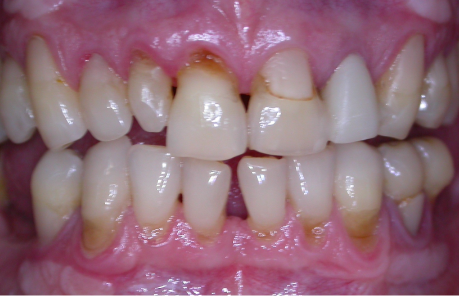
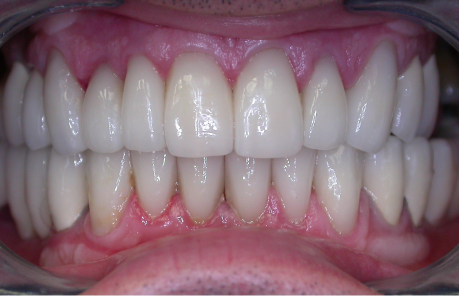
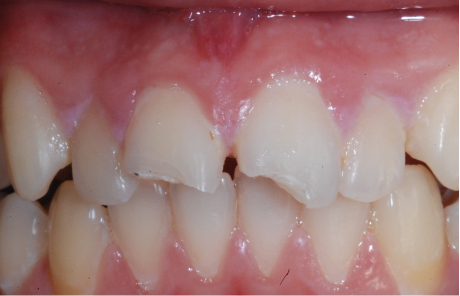
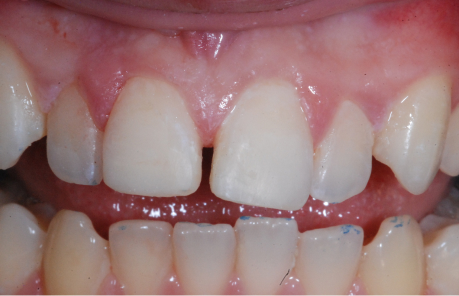
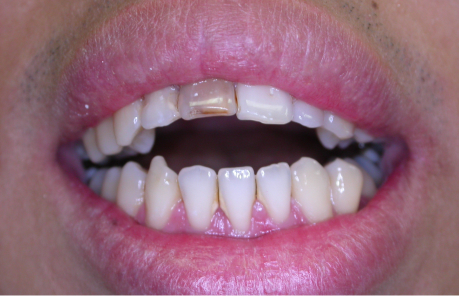
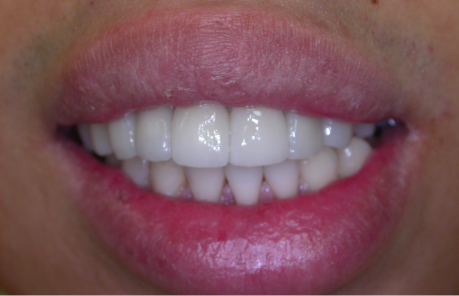
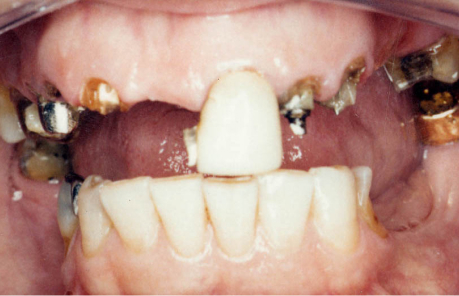
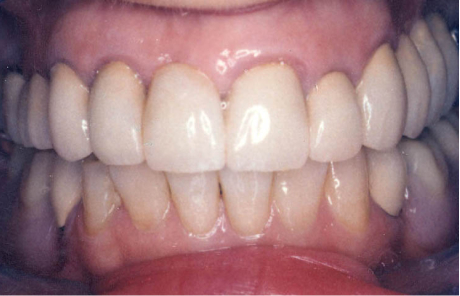
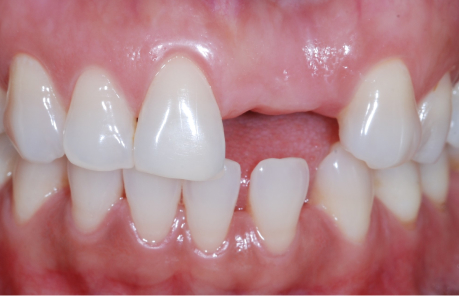
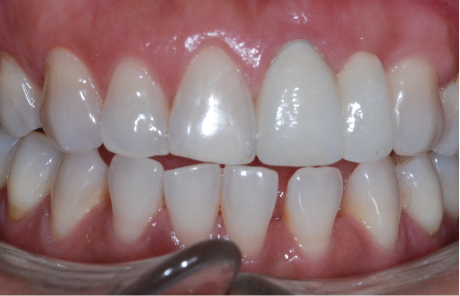
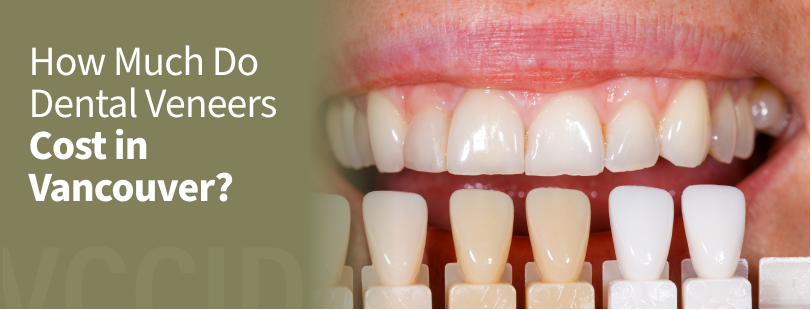
So, the first part of our seminar we’re going to talk about what happens when we lose teeth. I can break it down to about four categories. Number one, first of all, we have physical changes. Number two, we have cosmetic changes and that’s the result of what happens physically. Number three, we have functional changes as we lose teeth especially after we’ve lost several teeth, and then all three of these also have an impact on our self-esteem and psychological well-being.
Bone Atrophy Accompanies Tooth Loss
So, first of all, let’s look at physical. What happens when we lose teeth? Number one, what a lot of people don’t realize is when we lose teeth, we lose bone. The bone in the jaw will shrink when there’s no tooth. Just the analogy I can give you is our muscles. If we exercise, our muscles stay big and strong and as soon as we stop exercising, our muscles will start to shrink. The same thing happens in the mouth, but in this case, it’s not muscle that shrinks, it’s actually bone, and the bone will shrink in height and width, and it shrinks and continues to shrink throughout our lives.
If you know anybody who has dentures, they’ll say, “Well, my gums have shrunk so now my dentures are loose, and now I have to get them realigned.” Really in reality what’s happened, it’s not so much that the gums have shrunk, but the bone underneath has shrunk, and the gums have simply followed it. So it is true, the gums have shrunk, but it’s because the bone underneath has atrophied, In other words, it’s in disuse. It’s not being stimulated and it slowly starts to shrink.
And I can show that to you visually in these models here. This is a model of a lower jaw, and this is approximately an average size person, teeth and the height and width of bone that would be there. This first model here shows how much bone we lost after approximately one year if this person’s teeth were removed, and then, as the years go on this slowly progresses. In this case, here might be somebody who might be missing their teeth for 15 to 20 years, and this would be 25 to 30-plus years. As you can see the longer we’ve been missing teeth, the more the bone atrophies.
So, what’s the significance of this? Well, there’s a couple of things here, why this is so important, why this is so significant. Number one, if you take a look here there’s a couple of dimples here, and we all have that, that’s a little opening in the bone in the lower jaw, and out of that little opening, there’s a little vein and artery and a nerve. Normally, that’s far and away from the teeth as you can see here, but as the bone shrinks, eventually, that little opening, although it doesn’t change position, the bone on top shrinks and eventually that ends up on top of the ridge.
Decreased Denture Functionality
And you can imagine that somebody has a denture and it’s sitting on the ridge, when it gets to this point, anytime they bite, sometimes, it doesn’t have to be something hard it could be something even relatively soft, they’ll get a sharp jolt, because they’re literally pinching the nerve, and will get a sharp jolt that will run right up there, either to their chin or right up towards their ear. Also, along here in the lower jaw, there’s a lot of areas where the muscles attach. Muscles from the lip, muscles from the jaw or the cheek attach around here. Normally, they’re also far and away from the teeth, but once again, as this bone shrinks, it gets closer to the top of the ridge, and also, the denture starts to now press on some of those muscle attachments.
So, we can lose one or two teeth and adapt, we can still chew relatively well, but once we’ve lost all of our teeth, and we start to get this much atrophy it becomes a real issue. So, I have a number of people come in to see me who’ve had dentures for 15, 20, 25, 30 years, and now they’re coming in because they just can’t function anymore. They sometimes function better and easier with their teeth out than with their teeth in.
Tooth Loss in the Upper Jaw
The same thing happens in the upper jaw. What I showed you there was for the lower. This is an upper jaw. Same sort of thing. Here’s a full set of teeth, how much bone would be present after approximately one year, and then, maybe 5 to 10 years and then 15-plus years. Now we’re fortunate on the upper jaw because we have something here we call the hard palate, which is the roof of the mouth. It’s a different type of bone, different source, embryologically how it was formed, so it does not change.
It’s like a base-bone and it does not change. Just the bone where the teeth are, the bone that goes around the teeth. But the same thing happens to our upper jaw as we lose teeth. This bone shrinks in height and width. There is an opening here on our palate right behind our front teeth where there is a vein, an artery and nerve that exits there. In some cases, people find discomfort because their denture is pressing on there. There are some muscles attachments, now fortunately, they’re farther away on the upper then they are in the lower, but we do tend to have the same sort of problems, but not as much as on the bottom.
Tooth Loss in the Lower Jaw
On the lower, also we have the tongue and the floor of the mouth, which is constantly moving as we’re talking. So, on the bottom, when you have a full-lower denture you have something that looks like a horseshoe, and it’s sitting on a flat surface that’s as slippery as an ice rink. In Canada, hockey is our national sport, so of course, we compare everything to a hockey rink, and this thing tends to slide around like this. It’s not very comfortable, not very easy to function with. The upper is very similar except, the upper typically has a full-palate.
So, plastic will cover the entire roof of the mouth, so that we have a good, solid base, and also can provide a seal or suction so the denture does not drop down, but then that also affects our ability to taste and sense the texture of foods. So not only our ability to chew foods sometimes becomes impaired, but we also don’t taste the foods the same. We’ve got something foreign, plastic that absorbs tastes of old foods, develops a taste of its own, and also, we’ve basically lost ability to sense a texture of foods.
Decrease in Quality and Quality of Gum Tissue
So, those are the physical changes that occurs to the bone. There are other changes that occur. Number one, not only does the gum shrink in volume, so not only does the quantity change, but the quality changes. Normally, around all of our teeth is a very thick gum tissue. Just like the palms of our hands, and the souls of our feet, that tissue is designed to be able to withstand a toothbrush, food abrading against it, and to also provide a tight seal around our natural teeth.
When we lose a tooth, the gum shrinks and that volume of thick gum tissues shrinks, and if you take a look in the mirror at home, the gum tissue around your teeth is very pink, if you look at the gum tissue in your cheeks it’s so thin that you can see the blood vessels underneath, it’s not very well designed to provide a seal around teeth, nor is it well designed to support a denture sitting on top of it.
And so as time goes on, and we’re at the end-stage where we’ve lost a lot of bone, quality and quantity of gum tissue, now the gum tissue is not only sitting on a very small ridge, it’s also something that’s very loose, fragile, and very slippery. The other thing that happens is teeth start to shift and move.
How the Absence of One Tooth Effects the Others
We could lose one tooth, and it’s not so bad. We can still chew very well. You’ve got 28 to 32 teeth. It’s very hard to say if we lose 1 or 2 teeth that a person can’t function or chew well. It’s very easy for us to adapt, and that’s exactly what we do. We just take the food and move it to the other side. So we can lose 2 or 3 teeth and we have no problems being able to chew. However, that one tooth missing will cause shifting of the teeth adjacent, above it, and/or below it.
Teeth normally stand shoulder to shoulder, and it helps hold them in place, and the way our teeth fit together also helps hold them in place, but if we’re missing even one tooth, the one on the side, on either side, may start to shift. So teeth will start to tip, move. When they first come into the mouth as kids, they erupt very quickly because the roots are forming and they’ll break through the gums and come into contact in a matter of a few months and they’ll stop erupting or stop coming through when they make that contact.
As adults, our roots are fully develop so that process doesn’t happen actively, but it’s more of a passive movement whereas if this tooth was removed and there’s nothing here stopping this tooth, no tooth biting against it, it will slowly keep coming up and vice versa. A top tooth, if there’s nothing below it will slowly keep coming down, and eventually will start biting into the gums.
Redistribution of force
So, we can lose 1 or 2 teeth and still do quite well functionally, but it’s going to have implications 5-10-plus years down the road when our other teeth shift and it throws off our bite. So, it’s good and wise to do something preventive so that you don’t have other problems down the road. The other thing that happens as a result of losing teeth is the force that distributed on them changes.
Normally when we bite, our back teeth take the brunt of the force and much like a snowshoe, it’s spread across all of the teeth, and we lose 1 or 2 teeth, that’s not going to change the affect the forces have on the remaining too much, but if we’ve lost say a third to half of our teeth, the other ones that do remain take the brunt of the force, and then a number of things can happen. Teeth can start to shift and move as result of the excess force. We may find that teeth are not strong enough and teeth start to fracture because there’s more force on them, and the teeth are already weakened with fillings. So a whole variety of things can occur.
Bite Collapse
The other thing that happens is called bite collapse, and the best way I can describe that is when we open and close our jaw, our jaw rotates and in a joint just in front of the ear. So it opens and closes as we talk and as we eat, and what’s stops our jaw from closing is our back teeth, but if we’ve lost our back teeth or we’ve lost enough teeth that others have shifted then our bite starts to close up. And you’ll actually see, especially when we’ve lost all of our teeth, and people who have dentures, you’ll see that they’ve lost the stop that normally prevents their jaw from closing and their chin and nose will get closer together. We have something we call bite collapse.
In orthodontics, there’s a number of measurements that are done as far to determine how a person’s bite is, and if anyone of you is an artist, you’ll understand there’s symmetry in the human body, and generally, this is about one-third, this is about one-third and this is about one-third, but when we have bite collapse, this starts to scrunch up, and it actually will make up look much older.
The next thing that happens is…we’ve talked about changes in the bone, we’ve talked about changes in the gum tissue, we’ve talked about how forces are changed on the teeth, we also talked about how our bite changes.
Loss of Muscle Strength
We also have changes with our tongue. Normally, we have got teeth in place, and the tongue is kept kind of tight and scrunched up, but after we lose teeth that tongue tends to flatten out, it tends to lose its muscle tone. You may wonder what the significance of that is. The biggest significance comes when we have dentures because as much as people think dentures are held in place by suction or by a glue or an adhesive, especially on the lower jaw, those don’t work very well and if we lose muscle tone, our tongue is not as adapt being able to keep those lower denture in place.
Lastly, and I mentioned this a little bit as I went through the hard-tissue model here, there’s a number of nerves and muscles around the lower jaw, and as the bone shrinks those become exposed, they don’t become exposed, but they become much closer to the top of the ridge. They become much closer to where the edge of where the denture sits, and sometimes as we bite on these dentures, it starts to cause some discomfort, soreness in the either the muscle attachments or the nerves.